PERIODONTAL DISEASE OR PERIODONTITIS

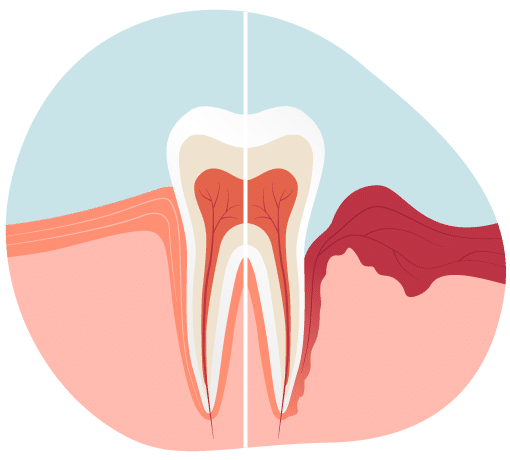
The supporting structures of the teeth, as the term suggests, provide support and stability to the tooth.
They include the periodontium—connective tissue and ligaments around the tooth, the cementum of the tooth, the gums, and the bone in which the teeth are anchored. Inflammation can quickly spread from one area to another.
To help you understand the mechanisms at play in this disease and how periodontal disease progresses through different stages, we will outline the main symptoms that can help you recognize and potentially prevent its onset.
Have you noticed your gums bleeding?
Sometimes gums bleed due to improper brushing techniques, brushing too hard, or using overly firm toothbrushes. However, this does not necessarily mean you have periodontal disease.
But if your gums bleed at the slightest provocation—when sucking between your teeth, touching them with a toothbrush, or eating—you should be concerned.
- Swollen gums.
- Bad breath is also associated with periodontal disease.
- Pain and numbness in the gums when biting or even without any stimulus.
- Tooth sensitivity to hot, cold, and sweet stimuli.
- Food getting stuck between teeth.
- Teeth shifting over time.
WHAT CAUSES PERIODONTAL DISEASE?
- Poor oral hygiene, food remnants, and plaque buildup are the primary causes.
- Genetic predisposition.
- Poor dental fillings.
- Misaligned teeth, crowding, and difficulty in cleaning.
- Malocclusion and teeth that are in premature contact, causing trauma.
- Poor prosthetic work, crowns, and bridges.
WHAT ARE THE RISK FACTORS FOR PERIODONTITIS?
Hormonal disorders, most commonly diabetes and thyroid diseases.

Certain medications that reduce saliva production.

Stress and smoking.
STAGES OF PERIODONTAL DISEASE

Swollen gums and bleeding at the slightest irritation are the first signs you may notice. If we recall that the primary cause of periodontitis is poor oral hygiene, food retention, and plaque buildup, we can also understand why gums begin to bleed.
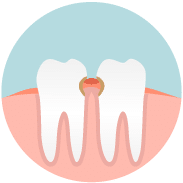
All bacteria in the mouth concentrate in dental plaque, causing both cavities and inflammation of the gum tissue around the teeth. This initial stage of periodontal disease is called GINGIVITIS. Gingivitis is characterized by swollen, red gums that bleed.
If we do not act when these early symptoms appear, the vicious cycle of periodontal disease begins.
Without proper oral hygiene, minerals from saliva deposit into the dental plaque, forming tartar. Dental tartar is a hardened deposit that cannot be removed at home.
In addition to containing microorganisms, tartar is rough and continues to exert mechanical pressure on the gums, disrupting circulation. Because of this mechanical pressure, the gums begin to recede, exposing the roots of the teeth, which become sensitive to hot and cold stimuli. This stage of periodontal disease is still reversible, as addressing the symptoms and causes can quickly restore oral health.
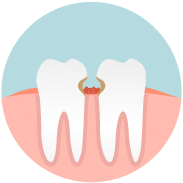
However, if this condition is neglected, spaces begin to form between the teeth, creating PERIODONTAL POCKETS as the fibers that hold the tooth in place deteriorate. As these pockets deepen, the disease progresses.
A periodontal pocket is the most important indicator of periodontal disease. It provides an ideal environment for the colonization of increasingly aggressive bacteria that further destroy the attachments and ligaments of the tooth-supporting structures.
IN THE ADVANCED STAGE OD PERIODONTAL DISEASE, bone destruction occurs, leading to tooth loosening and, ultimately, tooth loss.
HOW IS PERIODONTAL DISEASE TREATED?
Treatment can be conservative or surgical.
Conservative treatment involves ultrasonic tartar removal and gum cleaning. If you visit a dentist at this stage, periodontitis can be treated conservatively. However, if left untreated, periodontal pockets deepen, requiring aggressive curettage of the pockets, though still managed conservatively.
Surgical treatment—a flap surgery—is performed when periodontal pockets become extremely deep (over 4–5 mm). This indicates significant bone loss, which cannot be restored through conservative means.
Flap surgery is a routine procedure performed under local anesthesia. It involves making an incision in the gums, removing inflamed and granulated tissue from the pockets, and filling the spaces with artificial bone. To qualify for surgical treatment, periodontal disease must not be in its terminal stage—there must be sufficient remaining bone. This requires a clinical examination and an orthopantomogram (panoramic X-ray).
Postoperative recovery involves minimal pain, normal eating and drinking, and no swelling. Stitches are removed after 10 days.
Flap surgery offers numerous benefits, the most significant being prolonging the lifespan of your teeth and keeping periodontal disease in a stable phase.
Two months after flap surgery, prosthetic rehabilitation (crowns or implants) is typically initiated.
PREGNANCY AND PERIODONTAL DISEASE
There is a strong connection between periodontal disease and pregnancy.
You may have heard the saying: “I lost all my teeth during pregnancy.”
What is less known is that pregnant women should not be deprived of dental care during pregnancy. Visiting the dentist is not contraindicated—in fact, regular checkups, especially after the fifth month, are essential.
The issue is not with the teeth themselves, but with hormonal changes.

The hormones that significantly increase during pregnancy—estrogen and progesterone—are actually responsible for the development of certain problems, as they cause changes in the blood vessels of the gums.
If pregnant women have even a minor issue with gingivitis, it tends to progress during pregnancy under the influence of these hormones. The gums may bleed, become swollen and painful, making oral hygiene more difficult. Food often remains trapped in the pockets between the teeth, leading to tartar buildup. If such conditions are neglected, this can result in multiple cavities, periodontal disease, and eventually tooth loss.
It is also proven that untreated advanced periodontal disease increases the risk of preterm birth.
For pregnant women, checkups and cleaning of soft and hard deposits every two to three months are recommended. This keeps the oral cavity in good condition, and once hormones return to normal postpartum, the gums also stabilize without lasting damage.
PS. Periodontopathy is the leading cause of tooth loss and serves as a focal point from which other tissues and organs can become compromised. Unfortunately, periodontopathy cannot be completely cured, especially in cases where genetics play the most significant role. However, do not allow this disease to progress and cost you your healthy teeth.
Once periodontopathy has been diagnosed, whether it is treated conservatively or surgically, do not forget that regular check-ups with your dentist are crucial. This is the only way to keep the disease under control.
Although periodontitis is a disease caused by a combination of multiple factors, you are the one who can greatly influence its progression. Genetics is the only factor beyond our control, but everything else can be managed.
In today’s world, it is difficult to simply say, “reduce stress, quit smoking,” but keep in mind that these are major risk factors—not only for periodontitis but also for many other chronic and acute diseases.
You, together with us, can bring periodontopathy into a stable phase and keep your teeth for many years. The key to healthy gums and teeth is proper oral hygiene. As important as brushing technique is, regular tartar removal, replacing old crowns, and renewing old fillings are just as essential.
According to data, 65% of the population harbors pathogenic bacteria in their mouths that can lead to periodontopathy. If left untreated, these microorganisms enter the bloodstream and spread throughout the body.
FREQUENTLY ASKED QUESTIONS
Is periodontal disease treated surgically right away?
No, we opt for surgery only if conservative methods fail. It depends on the stage at which you visit the dentist.
Does flap surgery cure periodontal disease?
No. Periodontal disease has only slowed down and entered a kind of stable phase. However, with regular check-ups and by following your dentist’s advice on oral hygiene, the condition may remain stable for many years without worsening. If, after many years, periodontitis does become active again, another flap surgery is usually performed, all with the goal of preserving your teeth.
Does periodontal disease cause pain
No, except in acute phases. Common symptoms include bleeding gums, a sensation of fullness due to swelling, and food trapping.
If genetics is the main cause, the disease often progresses without pain—which is why regular dental checkups are crucial.
